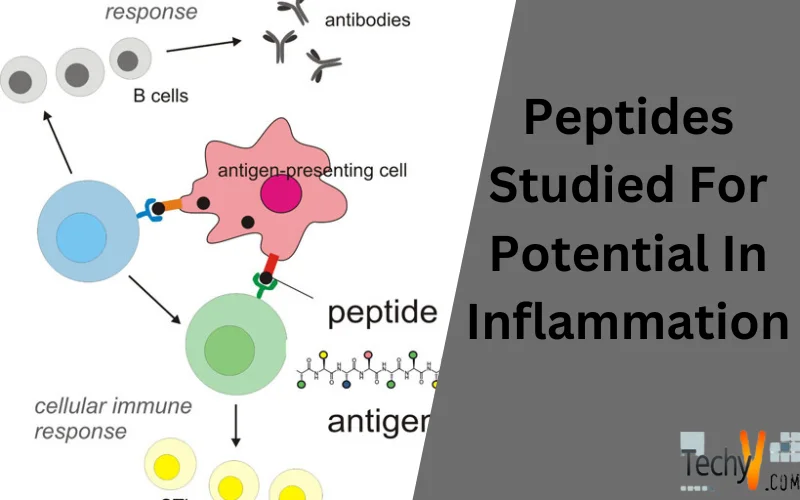
Unlike natural analogs, synthetic anti-inflammatory peptides tend to be smaller and more selective in their impact. Studies suggest that natural anti-inflammatory peptides, such as -MSH, may play an important role in the intricate control of the immune system. Unfortunately, excessive inflammatory reactions or some disease processes might overwhelm or render non-functional natural mechanisms. This is why researchers are keen to create peptides that may quell inflammation. Take a peek at peptides’ present and potential future in cases of inflammation.
Peptides And Inflammation
Inflammation is an essential immunological reaction that aids in recovery from injury, infection, or other potentially damaging stimuli. A chain reaction of immunological reactions must be set in motion to stop the bleeding, eliminate the infection, and begin the healing process. However, when inflammation gets out of control, it causes problems. Listed below are a few examples of this.
Chronic inflammation results if an immune reaction does not fade when it should or if the damage keeps returning after the immune system has already dealt with it. Inflammation that lasts for weeks, months or even years is called chronic. Rheumatoid arthritis, IBD, and cardiovascular disease are a few examples of chronic conditions that may develop from chronic inflammation.
While inflammation’s primary function is tissue protection, it may also cause harm if it persists for too long. This may happen when immune cells assault tissues directly or when free radicals and inflammatory cytokines are produced. ROS refers to oxygen molecules that undergo chemical reactions. While reactive oxygen species (ROS) are essential for many physiological functions, including cell communication and host defense against pathogens, too much of a good thing may be harmful. When talking about antioxidants, the goal should be to reduce reactive oxygen species (ROS). It has been hypothesized that peptides that may reduce inflammation might also be powerful antioxidants.
While inflammation may manifest locally, it may spread if not mitigated. Muscle atrophy and fever may result from systemic impacts. Furthermore, it may lead to organ dysfunction and promote the development of systemic disorders.
In a strange twist, acute inflammation is essential for normal tissue repair, but persistent inflammation might impede it. Prolonged inflammation may impede the restoration of normal tissue structure and function by delaying the repair and remodeling processes. The immune system’s ability to switch gears from the inflammation required to eliminate pathogens to the kind of immune response that heals injured tissue is hypothesized to be potentially aided by several peptides, which might also aid in initiating the healing process.
BPC 157 Peptide
The synthetic peptide BPC-157, based on a protein found in stomach acid, has suggested a positive impact in accelerating tissue regeneration and healing in several animal models. Studies on its impact on gastrointestinal illness, tendonitis, and cardiovascular disease are extensive. Pro-inflammatory cytokines, such as tumor necrosis factor-alpha (TNF-alpha) and interleukin-6 (IL-6), have been speculated to be suppressed by BPC-157. The nuclear factor kappa B (NF-kappaB) pathway, important in controlling inflammation, has also been purported to be suppressed. It has been speculated that BPC-157 may reduce inflammatory gene expression through blocking NF-kappaB.
By decreasing the levels of oxidative stress indicators, including nitric oxide and malondialdehyde (MDA), BPC-157 has been suggested to exert antioxidant potential as found in certain animal studies. Damage to cells results from oxidative stress, which happens when antioxidant defense systems are overwhelmed by the creation of reactive oxygen species (ROS). Reducing the creation of reactive oxygen species in the gastrointestinal tract is one way that BPC-157 is purported to fight oxidative stress.
GHK-Cu Peptide
Short peptide GHK-Cu comprises the copper-binding amino acids glycine, histidine, and lysine. Epigenetic alterations have been suggested to affect gene expression in mice given GHK-Cu. These alterations have been speculated to lessen inflammation, speed up the recovery of damaged tissues, and improve the efficiency of internal systems that flush out cellular waste and toxic byproducts of metabolism.
LL-37 Peptide
LL-37 belongs to the family of antimicrobial peptides (AMPs) and is a cathelicidin peptide. The innate immune response to microbes involves producing a wide variety of peptides called cathelicidins.
Studies suggest that beyond its potential antibacterial impact, the possible uses of LL-37 have attracted much interest. It has been hypothesized that LL-37 may significantly involve several biological processes and substantial antibacterial activities against various pathogens. In autoimmune illnesses like rheumatoid arthritis, LL-37 has been speculated to help regulate inflammation. As research suggests, It may affect the onset and course of autoimmune illnesses due to its potential in regulating immune cell activity and cytokine production.
Sermorelin Peptide
Investigations purport that inflammation may be mitigated through Sermorelin and other analogs of growth hormone-releasing hormone. Researchers suggest these peptides may potentially suppress the inflammatory cytokines responsible for poor wound healing, scarring, and even heart dysfunction, suggesting that they might alter cytokine signaling. Studies have suggested that Sermorelin may be the most “effective” anti-aging peptide within the context of animal experiments, possibly reducing inflammatory reactions and increasing antioxidant activity.
Buy peptides online only if you are a scientist researching these compounds in a controlled laboratory environment.
References
[i] K. Škrlec et al., “Engineering recombinant Lactococcus lactis as a delivery vehicle for
BPC-157 peptide with antioxidant activities,” Appl. Microbiol. Biotechnol., vol. 102, no. 23,
pp. 10103–10117, Dec. 2018, doi: 10.1007/s00253-018-9333-6.
[ii] D. B. Richards and J. M. Lipton, “Effect of alpha-MSH 11-13 (lysine-proline-valine) on
fever in the rabbit,” Peptides, vol. 5, no. 4, Art. no. 4, Aug. 1984, doi: 10.1016/0196-
9781(84)90027-5.
[iii] T. Brzoska, T. A. Luger, C. Maaser, C. Abels, and M. Böhm, “Alpha-melanocyte-
stimulating hormone and related tripeptides: biochemistry, antiinflammatory and protective
effects in vitro and in vivo, and future perspectives for the treatment of immune-mediated
inflammatory diseases,” Endocr. Rev., vol. 29, no. 5, Art. no. 5, Aug. 2008, doi:
10.1210/er.2007-0027.
[iv] T. A. Luger and T. Brzoska, “α‐MSH related peptides: a new class of anti‐inflammatory
and immunomodulating drugs,” Ann. Rheum. Dis., vol. 66, no. Suppl 3, Art. no. Suppl 3,
Nov. 2007, doi: 10.1136/ard.2007.079780.
[v] S. Khaleghi, J. M. Ju, A. Lamba, and J. A. Murray, “The potential utility of tight junction
regulation in celiac disease: focus on larazotide acetate,” Ther. Adv. Gastroenterol., vol. 9, no.
1, Art. no. 1, Jan. 2016, doi: 10.1177/1756283X15616576.
[vi] S. Gopalakrishnan et al., “Larazotide acetate regulates epithelial tight junctions in vitro
and in vivo,” Peptides, vol. 35, no. 1, Art. no. 1, May 2012, doi:
10.1016/j.peptides.2012.02.015.
[vii] S. Gopalakrishnan, A. Tripathi, A. P. Tamiz, S. S. Alkan, and N. B. Pandey, “Larazotide
acetate promotes tight junction assembly in epithelial cells,” Peptides, vol. 35, no. 1, Art. no.
1, May 2012, doi: 10.1016/j.peptides.2012.02.016.
[viii] M. Storr, “[Larazotide as an option in case of failure of a gluten-free diet],” Med.
Monatsschr. Pharm., vol. 39, no. 2, Art. no. 2, Feb. 2016.